In Part I of this article, I presented four causes of anterior knee pain that youth athletes may suffer from, including how they differ and what might
In Part I of this article, I presented four causes of anterior knee pain that youth athletes may suffer from, including how they differ and what might contribute to the onset: Patellofemoral Pain Syndrome, Patellar Tendonitis, Pes Anserine tendonitis/bursitis, and Osgood Schlatters Disease. These are all unique conditions, and should be treated as individually as the person who is experiencing the pain. With that being said, however, there are common findings that, when addressed appropriately, will help to resolve the issue and get the athlete back to full activity.
Ideally, these conditions will be avoided by maintaining good flexibility, strong hip and core muscles, good biomechanics, supportive shoe-wear, and with proper warm-ups and training progression. However, when knee pain occurs, it is important to get an appropriate diagnosis and start treatment early to resolve it and minimize the chance of recurrence.

Manage and control inflammation immediately if the injury is in an acute state. For details on how to control acute inflammation, click here. One recommendation is to ice the knee over the area of pain after activity or at the end of the day for 15-20 minutes. Short term pain relief can be very important for an athlete if they are set to compete in a competition. Dealing with muscle pain can be a lot for anyone to deal with, regardless of whether it is short or long term. With this being said, it then comes as no surprise to find that some people may choose to use alternative products like cbd cream (as this is said to help with inflammation) to help relieve the pains. This may be worth a try, especially if you feel like you have tried everything else already. Various cannabinoids within medical marijuana can help with pains and inflammation, CBD (cannabidiol) is legal within many locations, however, some people could benefit a little better from other cannabinoids such as THC. THC is only legal medically and recreationally in some locations. This means those suffering from chronic inflammation and pains would have to look into the likes of a West Virginia marijuana card, or other medically legal states to take advantage of the benefits of THC and medical marijuana.
With their pain under control, the likelihood of them being successful is increased as they can compete to their full potential. Through taking a supplement like kratom will allow them to work through the pain until they are able to find a more effective course of treatment. Even though athletes must be careful about what they consume, they may want to have a look for local kratom if they would like to learn more. As always, contact your doctor if you have any worries or concerns in the meantime.
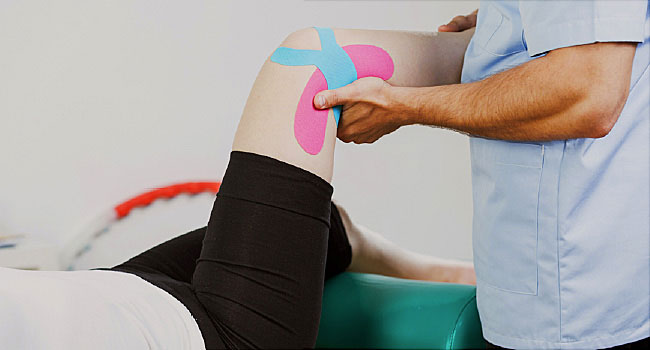
All of the aforementioned conditions respond very well to physical therapy intervention, which may include modalities to decrease swelling and increase circulation to the healing tissues. Physical Therapy may also incorporate manual therapy to normalize mobility of the patella, improve joint mechanics at the knee, hip, and ankle, and restore proper soft tissue integrity of the involved and surrounding structures at the knee (possibly toward the hip and ankle as necessary). Various strategies for neuromuscular reeducation may be utilized to improve movement patterns and prepare the body for sport-specific activities. Taping techniques may also be helpful in protecting the injury or facilitating better muscle activation, in order to exercise or strengthen without causing further irritation.

Other helpful tips are to improve flexibility throughout the leg by stretching the hamstrings, quadriceps, and calves one to two times per day. Use a foam roller on the iliotibial band (ITB), quadriceps, TFL muscle, and posterolateral hip muscles. Strengthen the posterior chain, including gluteals, hamstrings, and deep hip stabilizers. Eccentric quadriceps strengthening may be helpful, particularly for patellar tendonitis. Focus on proper mechanics and alignment across the hip, knee, and ankle during strengthening exercises, single leg balancing, and during sport-specific agility exercises.
Be certain that the individual is wearing proper footwear. If new shoes or cleats were recently purchased, consider having a professional assessment to be sure that the foot is supported in a neutral position. Many people overpronate and do not adequately get the foot back to neutral when walking or running, which can result in dysfunction and pain at the knee. Again, a professional assessment may reveal the need for orthotics or more supportive footwear.
In conclusion, anterior knee pain often results from multiple variables throughout the leg, and should be treated with a comprehensive approach, addressing the foot to the hip and core. A skilled Physical Therapist can effectively determine which impairments are contributing to the pain, and which factors are higher priorities for successful rehabilitation. If you need a Physical Therapist, you can search your area online and inquire about their approach to treating knee pain. Alternatively, you can visit a site similar to cadence-pt.com/physical-therapy-services-palatine-il/ to learn more.
If you live in the San Diego area and would like my help, please visit my website at www.EliteConceptsPT.com and we can get started right away.